Often Overlooked But In Need Of Attention: Gynecological Care For Trans Men
When it comes to healthcare, discussions around gender identity and reproductive health have often been overlooked or relegated to the sidelines. Trans men, in particular, face a unique set of challenges in navigating their healthcare needs, including gynecological care.
This blog aims to shed light on the often neglected but critical aspects of gynecological care for trans men.
We’ll cover various topics, from breast tissue health to surgical options, providing an easy-to-understand guide for those seeking to take charge of their well-being.
Breast Tissue Health For Trans Men
Breast tissue health is a crucial concern for trans men, especially those who haven’t undergone top surgery.
It involves being aware of any family history of breast cancer, regularly examining and becoming familiar with the look and feel of your breasts, and considering cancer screening such as mammograms and ultrasounds.
This proactive approach helps in the early detection of any abnormalities or changes, ensuring that breast health is monitored and maintained.
Whether you opt for surgery or not, taking care of your breast tissue is an essential aspect of gynecological care for trans men, promoting overall well-being and peace of mind.
Breast health is a crucial aspect of gynecological care for trans men, especially if there is a family history of breast cancer.
Here’s what you should consider:
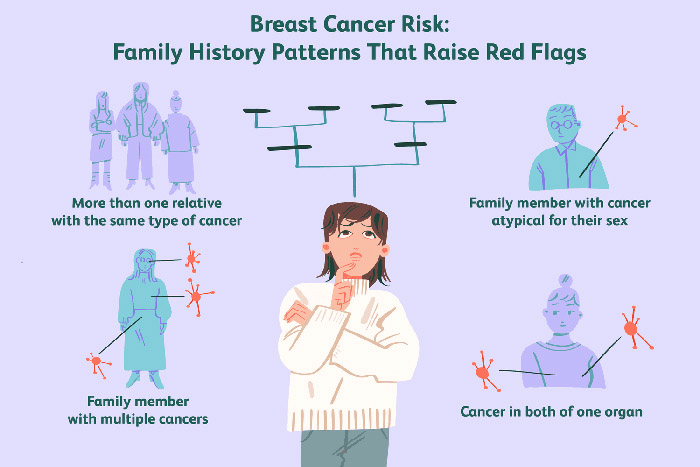
Has A Member Of Your Family Had Breast Cancer?
Start by discussing your family medical history with a healthcare provider.
If there’s a history of breast cancer, you may need more frequent breast examinations or screening.
Familiarize Yourself With The Look And Feel Of Your Breasts
Trans men who have not had top surgery should become acquainted with their breast tissue.
Regularly check for unusual changes, such as lumps, redness, or skin changes.
Being proactive in monitoring your breast health is essential.
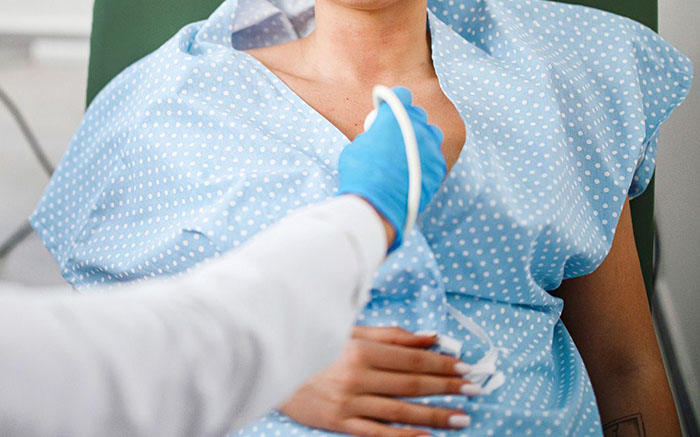
Cancer Screening For Trans Men
Regular breast cancer screening is a key part of gynecological care for trans men.
Mammograms, ultrasounds, and breast self-exams help detect any potential issues early, increasing the chances of successful treatment.
Pelvic Health For Trans Men
Pelvic health is a fundamental component of gynecological care for trans men.
Even though their reproductive organs may differ, it’s essential to maintain pelvic well-being.
Regular self-examinations help detect any discomfort or abnormalities.
While traditional gynecological exams may not be needed, general pelvic exams should be considered and tailored to individual health needs.
Pap smears might not be applicable, but discussing alternative screenings with your healthcare provider is crucial.
Routine screenings for sexually transmitted infections (STIs) play a vital role in ensuring overall pelvic health.
By staying proactive and informed, trans men maintain their pelvic health and overall well-being.
While gynecological care for trans men may not involve reproductive organs, it’s essential to maintain overall pelvic health.
Here are some important aspects to consider:
Inspection Measures For Trans Men
Regularly examine your pelvic area for any signs of discomfort, swelling, or abnormalities.
If you notice anything unusual, consult with a healthcare provider.
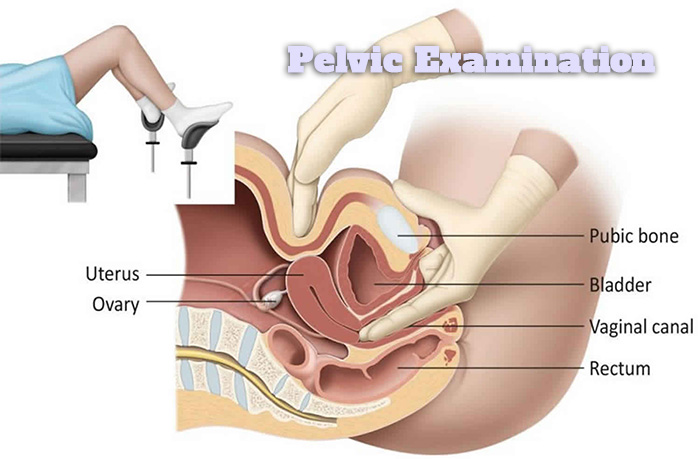
Pelvic Examination
Trans men might not require traditional gynecological exams, but a general pelvic exam helps identify any issues related to the pelvic region.
Talk to your healthcare provider about the appropriate frequency of these exams.
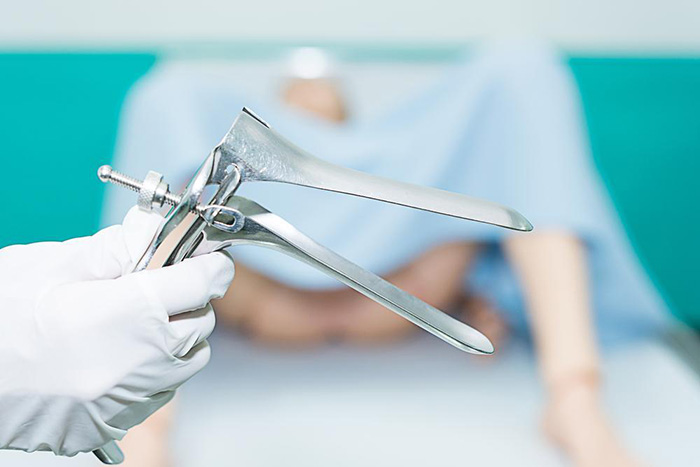
Pap Smear
Pap smears are typically done to screen for cervical cancer, which is not a concern for trans men.
However, it’s essential to discuss the need for any alternative screenings or tests based on your individual health needs.
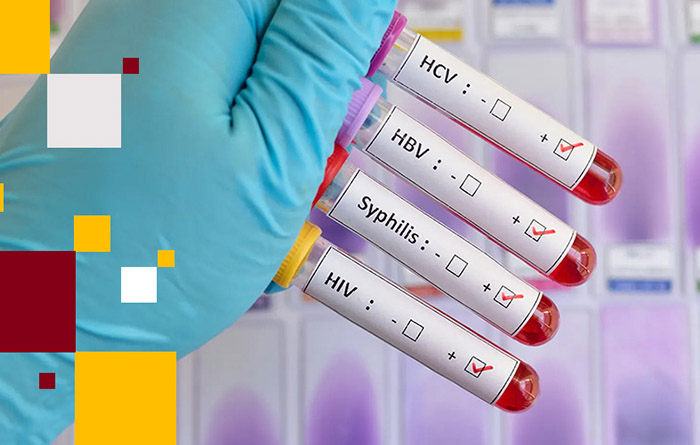
Sexually Transmitted Infections Screening
Regular screenings for sexually transmitted infections (STIs) are crucial for maintaining pelvic health.
Ensure you’re getting tested for STIs as recommended by your healthcare provider.
What Trans Men Need To Do To Stay Healthy
Maintaining sexual health is paramount, whether you’re sexually active or not.
Here’s what you need to consider:
Use Condoms Or Other Protection
If you engage in sexual activity, using condoms or other forms of protection is vital to reduce the risk of STIs and unwanted pregnancies.

Get Yourself And Your Partner Tested
Both you and your partner should get regular STI screenings to ensure that any infections are detected and treated promptly.
Take Steps To Prevent HIV
HIV prevention is a critical component of gynecological care for trans men.
PrEP (pre-exposure prophylaxis) and safer sex practices help reduce the risk of HIV transmission.

Get Vaccinated
Ensure you’re current on vaccinations for preventable STIs, such as HPV and hepatitis B.
Know The Risks Of Sexual Activity
Understanding the risks associated with sexual activity, including how to prevent unwanted pregnancies and the transmission of STIs, is vital for your sexual health.
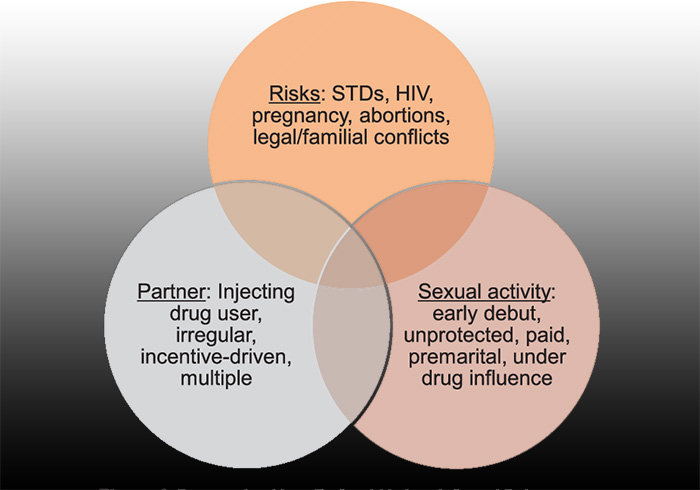
Safer Sex
Practicing safer sex involves using protection, regular testing, and open communication with your partner(s).
Make it a priority to engage in safe and consensual sexual activity.
Contraceptive Program For Trans Men
Even though trans men may not require contraception to prevent pregnancy, some contraceptive methods are beneficial for other reasons, such as managing hormones or controlling menstruation.

Here are a few options to consider:
Barrier Methods
Barrier methods like condoms and dental dams are essential for preventing the transmission of STIs.
These are used to reduce dysphoria during sexual activity.
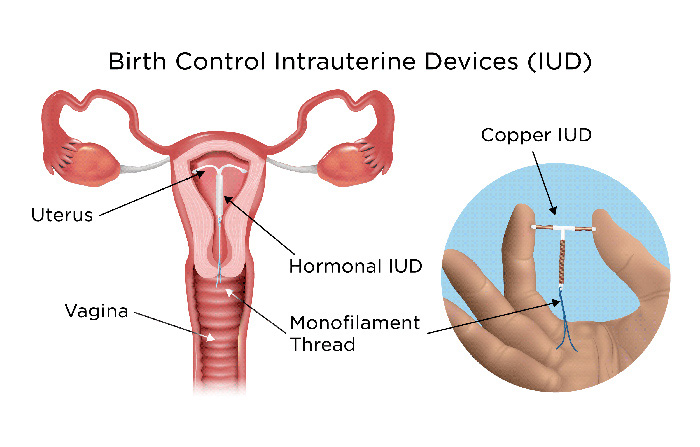
Intrauterine Devices (IUDs)
While IUDs are primarily used for birth control, they help manage menstruation for trans men.
Discuss this option with your healthcare provider.
Hormonal Contraception
Hormonal contraceptives, like birth control pills, patches, or injections, are not typically prescribed for trans men as a primary form of contraception.
However, they may be used to manage menstruation or hormone-related issues.
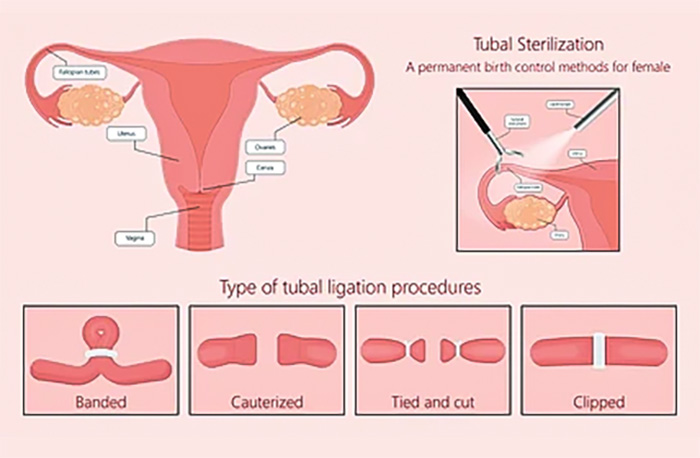
Permanent Contraception
For those who are certain they do not want to have children in the future, permanent contraception options like tubal ligation are considered, as they offer peace of mind.
Stopping Menstruation: Testosterone Use For Trans Men
Many trans men on hormone therapy experience changes in their menstrual cycle.
Testosterone therapy often leads to amenorrhea (the absence of menstruation).
If this is a goal, consult your healthcare provider to discuss the right hormone regimen.
Body Image For Trans Men
Gynecological care for trans men also encompasses emotional well-being.
Addressing body image concerns that may arise as you transition is essential.
Seek support from healthcare professionals and mental health specialists to navigate these feelings.

Use Of Male Gender Equipment For Trans Men
Using male gender-affirming items, including clothing and prosthetics, plays a significant role in helping trans men feel more comfortable and aligned with their gender identity.
These items enhance their self-esteem and overall well-being by allowing them to express their identity authentically and comfortably.
Many trans men use male gender equipment to affirm their gender identity and feel more comfortable in their bodies.

Here are some common options:
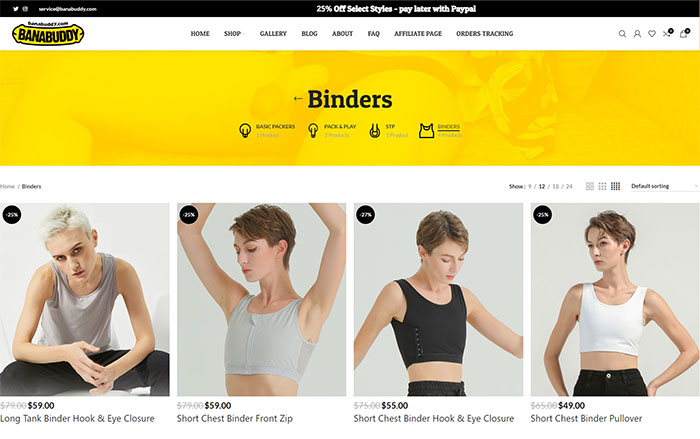
Binder
Binders are compression garments that flatten the chest and create a more masculine appearance.
Choosing a binder that fits well and doesn’t cause discomfort or breathing difficulties is important.
We recommend checking out these binders.
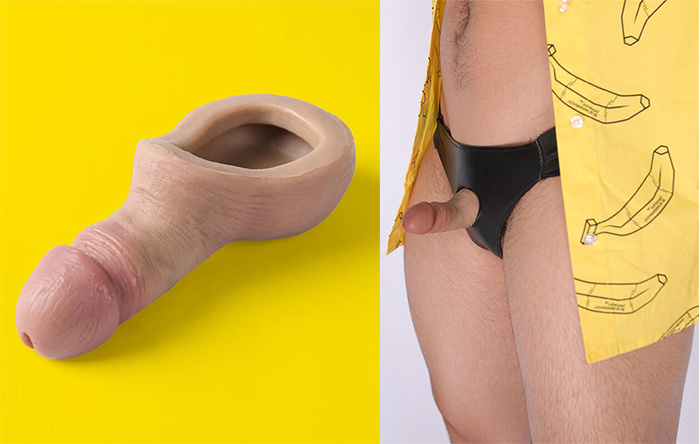
Packer
A packer is a prosthetic device that creates the appearance of male genitalia.
Selecting the right packer for your comfort and lifestyle is crucial. Check out this Packer.

STP (Stand-To-Pee)
STP devices enable trans men to urinate while standing.
Finding an STP that suits your needs and preferences is essential for daily comfort.
Take a look at this STP here.
Surgery Or Hormone Therapy For Trans Men
Surgery and hormone therapy are transformative steps in a trans man’s journey to align their physical appearance with their gender identity.
These choices are highly personal, and consulting with medical professionals is essential to ensure that these choices resonate with personal aspirations and necessities.
For some trans men, gender-affirming surgeries and hormone therapy are essential steps in their transition.
Here are some common options:
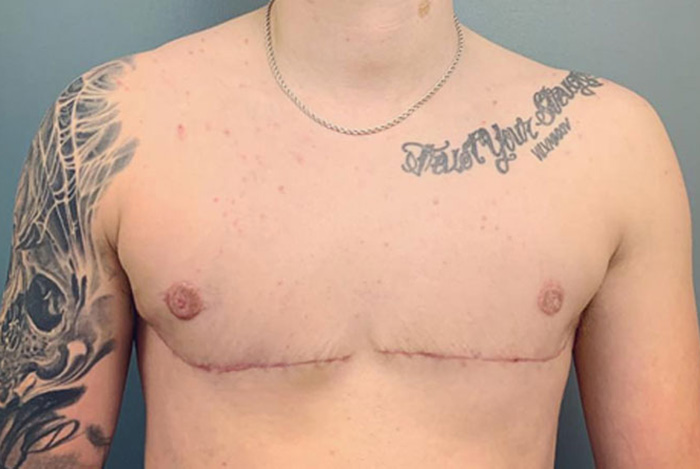
Top Surgery
Top surgery involves chest masculinization and may include mastectomy or breast reduction.
It is a significant step in achieving a more masculine appearance.
This transformative surgery is a significant step in the journey of many trans men to align their physical and gender identities.
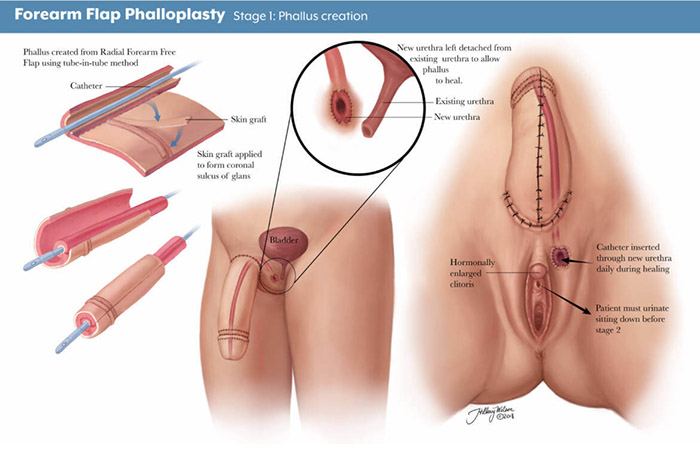
Bottom Surgery
Bottom surgery encompasses a variety of gender-affirming procedures for trans men, including metoidioplasty and phalloplasty, to create male genitalia.
These elective surgeries are tailored to align one’s physical self with their gender identity, enhancing overall well-being and self-assurance.
Penile Plasty
Penile plasty is a surgical procedure sought by some trans men as part of their gender-affirming journey.
It involves the creation of a neophallus, a penile-like structure that enhances both appearance and functionality.
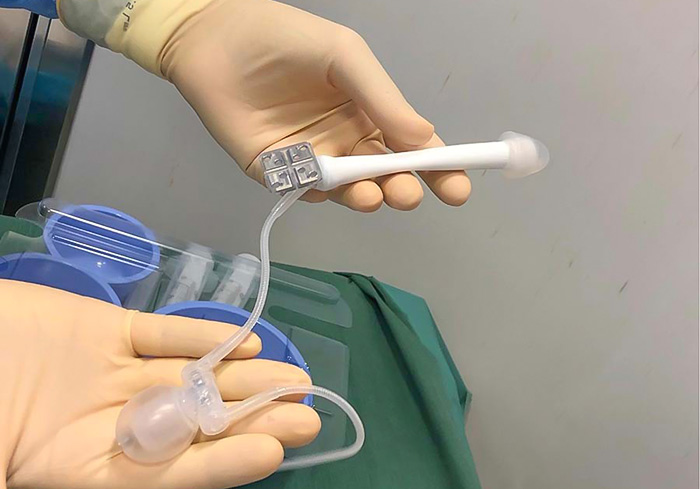
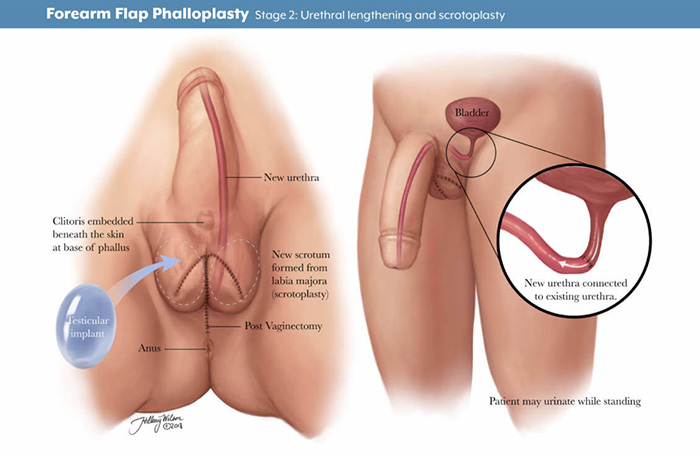
Scrotoplasty
Scrotoplasty is a gender-affirming surgical procedure, often part of bottom surgery for trans men.
It involves the creation of a scrotum, a vital component in achieving a more complete male genital appearance.
This elective surgery contributes significantly to trans man’s journey towards aligning their physical body with their affirmed gender identity, enhancing their self-confidence and well-being.
It is performed as part of bottom surgery or separately.
It’s a personal choice that reflects an individual’s unique gender-affirming path.
Conclusion
Gynecological care for trans men is a complex and multifaceted aspect of healthcare.
It encompasses various factors, from breast tissue health and sexual health to body image and surgical options.
It’s important to prioritize your well-being and work closely with healthcare providers who understand your unique needs.
By addressing these often-overlooked aspects of healthcare, trans men navigate their journeys with confidence, ensuring their overall health and emotional well-being are in focus.
Remember that your healthcare decisions should always align with your personal goals and preferences, and there is no one-size-fits

 Basic Packers
Basic Packers Pack & Play
Pack & Play STP
STP